Support Pathways of Care for Traumatic Injuries (PACE-TRI)

Closing the gap between emergency and recovery
Every year, tens of thousands of Australians experience so-called “mild” head and neck injuries such as whiplash and concussion. But mild does not mean minor. Without early diagnosis and coordinated care, up to half will develop persistent pain, cognitive impairment, psychological distress and disability that can last months, years or a lifetime. Pathways of Care for Traumatic Injuries (PACE-TRI) is transforming how these injuries are identified, treated and supported – closing the gap between emergency care and recovery.
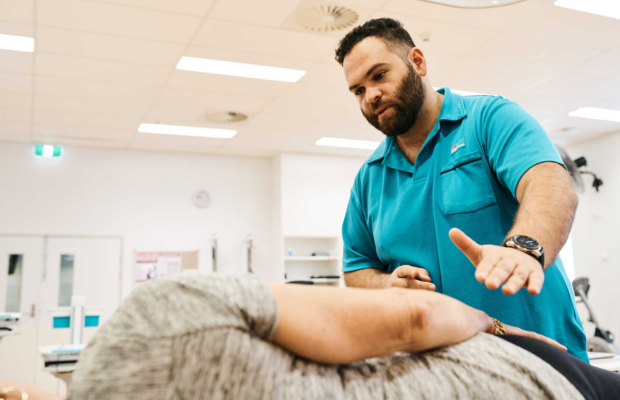
PACE-TRI delivers early, integrated care for people with whiplash and concussion – injuries that are common, disruptive and frequently overlooked. By ensuring assessment within 10 days and bringing neurology, neuropsychology, nursing and physiotherapy together in a single consultation, PACE-TRI replaces fragmented referrals with one clear pathway and a personalised recovery plan.
Your support will:
- Ensure early assessment within 10 days – not months
- Prevent long-term disability through coordinated care
- Identify psychological distress early, including PTSD
- Reduce avoidable emergency department re-presentations
- Create a scalable national model of trauma care
“With the right care in the critical early window, concussion and whiplash should not be a lifelong problem.”
– Dr Vincent Oxenham, Senior Clinical Neuropsychologist, Royal North Shore Hospital
Mild injuries. Life-altering consequences.
Tens of thousands of Australians
Around 30% of whiplash patients
Around 20% of adults with concussion
These injuries are often invisible and difficult to diagnose.
In busy emergency departments, whiplash and concussion are typically classified as “mild” and non-urgent; while life-threatening injuries are ruled out, the underlying drivers of long-term pain, cognitive impairment and psychological distress are frequently missed. Patients are often discharged without a clear follow-up plan and enter long, costly and ineffective referral pathways that delay recovery and compound harm. Care becomes fragmented as people move between emergency departments, GPs, imaging services and specialists, often undergoing unnecessary tests that fail to address the true causes of their symptoms.
Without early screening and coordinated care, pre-existing mental health issues and ongoing psychological distress – including conditions such as PTSD – are often missed, allowing chronic symptoms to develop and derail work, study, relationships and quality of life.
A model of care that works
PACE-TRI is a proven, evidence-based model designed to deliver the right care at the right time. It is built on two simple but powerful principles: early assessment within 10 days of injury, and multidisciplinary care delivered together, not in isolation.
Pillar 2: Multidisciplinary Care
Pillar 3: Coordinated Recovery Pathways
“We are creating a model of care that seems like a no-brainer but doesn’t actually exist yet.”
– Dr Vincent Oxenham, , Senior Clinical Neuropsychologist, Royal North Shore Hospital

Help change the future of trauma care.

‘I finally felt believed.’
After a cycling accident, Dannielle was told everything looked fine. But she struggled with brain fog, memory loss and constant pressure in her head. Through the PACE-TRI model at the Royal North Shore Hospital Concussion Clinic, she was assessed by a multidisciplinary team, given a tailored plan and supported back to recovery.
“Seeing three specialists together was invaluable. I finally felt believed – and I started getting better.”
– Dannielle Glasgow, competitive cyclist
What your support makes possible
Your support will help scale PACE-TRI across six emergency departments in New South Wales and Queensland, embedding early screening, training clinicians and building sustainable care pathways. This work has the potential to improve outcomes for more than six million Australians.
At Royal North Shore Hospital, this approach is already delivering results:
- Over 90% of patients recover within two clinical visits
- Marked reductions in emergency department re-presentations
- Faster, safer return to work, school and sport
Funding overview:
Total investment needed: $2.9M over 5 years

Related Stories

A vision for cancer care – NORTH STAR VNP Cancer Clinical Trials Showcase highlights innovation and progress
Read more
MEDIA RELEASE – Introducing Australia’s premier cancer clinical trials centre NORTH Sydney Trials and Research Van Norton Poche (NORTH STAR VNP)
Read more