Help create the Adaptive Platform for Sepsis Care

Help stop the clock on sepsis
Sepsis is one of the world’s most urgent and under‑recognised medical emergencies. It can kill within hours, and every hour treatment is delayed increases mortality by up to 9%. At Royal North Shore Hospital, intensive care specialists are launching the Sepsis Adaptive Platform – a connected model spanning early detection, rapid treatment, and long‑term recovery, powered by a Single Digital Patient Record.
Your support will help us detect sepsis earlier, deliver the best treatments faster, and support survivors for the long haul. The Sepsis Adaptive Platform tackles the full spectrum of sepsis care: from recognising danger sooner, to learning which treatments work best for each patient, to ensuring survivors are supported months and years after hospitalisation.
Your gift will:
- Accelerate real‑time detection and clinical alerts
- Expand adaptive clinical trials across NSW
- Reduce deaths, disability, and hospital readmissions
- Build integrated rehabilitation services for sepsis survivors
- Share a scalable model nationally and internationally
“There is no magic bullet for sepsis, yet. Improving the treatments we have in the ICU will provide the best chance of improving survival of patients with sepsis.”
– Associate Professor Naomi Hammond – Executive Director of Research, Northern Sydney Local Health District
Sepsis: a silent killer, hiding in plain sight
1 in 5 global deaths
84,000 Australians each year
Up to 9% higher mortality
Sepsis is the body’s extreme response to infection, triggering organ failure and death if not treated fast. Mortality rises for every hour treatment is delayed, and around 35% of all in‑hospital deaths involve sepsis. Survivors often face disability, cognitive decline, PTSD, and frequent readmissions – with up to 70% readmitted within a year.
Care is fragmented. Patients move between GPs, Emergency Departments and hospitals, while vital information sits across separate systems – causing delays that can be deadly. And after discharge, survivors often face a maze of services with no unified recovery pathway.
A new approach to saving lives
To combat this deadly disease, our specialist sepsis research team at Royal North Shore Hospital is launching the Sepsis Adaptive Platform – a connected program transforming how we detect, treat, and support sepsis patients.
Pillar 2: Adaptive Platform Trial
Pillar 3: Physical & Mental Rehabilitation
“With sepsis we want to find the best ways of supporting people’s vital organ function… and then integrate those treatments.”
– Associate Professor Anthony Delaney – Senior Staff Specialist, Intensive Care Unit, Royal North Shore Hospital
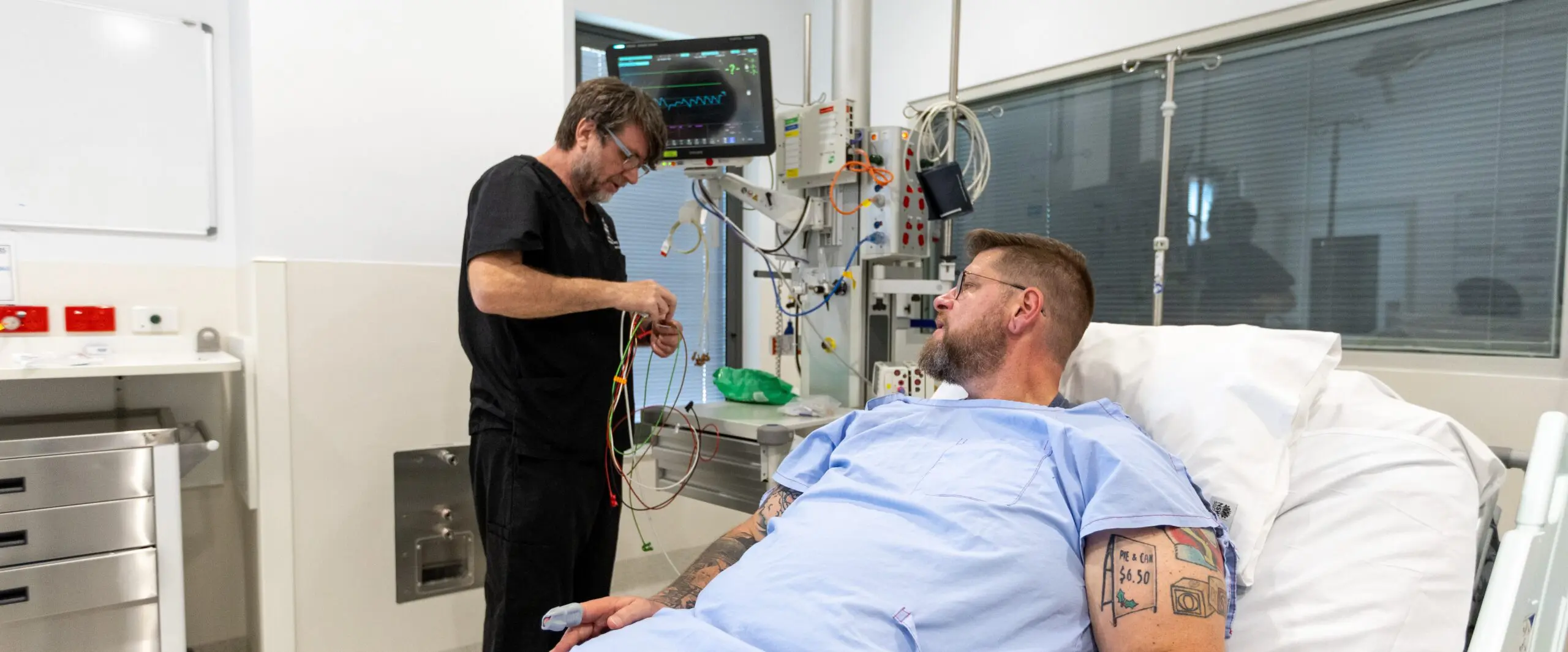
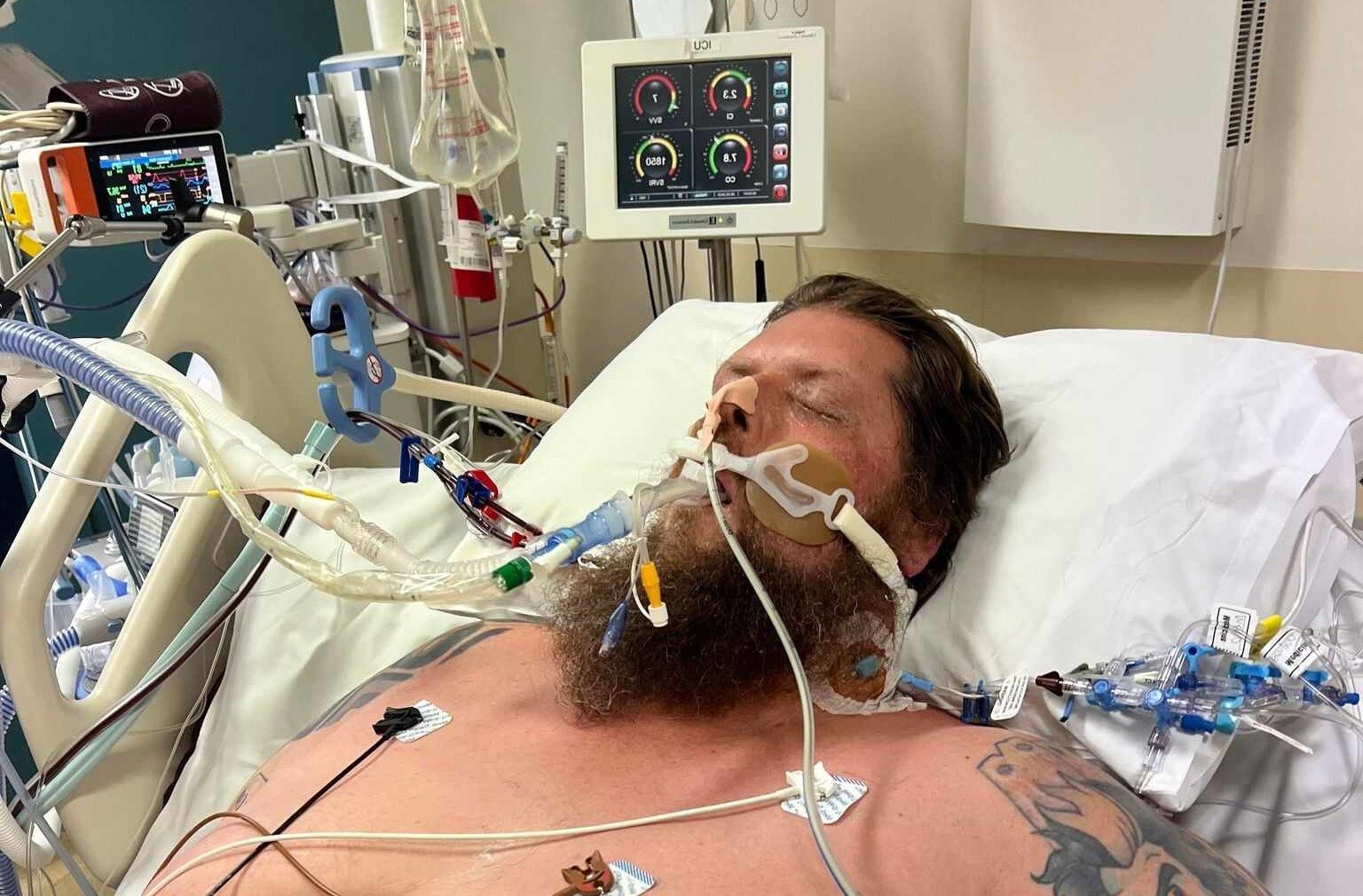
“It changed my life entirely.”
A small puppy scratch led to septic shock and multiple organ failure. Jacob Dye spent weeks in intensive care and months in recovery. Like many survivors, he experienced lasting physical and psychological impacts – and now, as a senior researcher, he is helping shape the future of sepsis care through this program.
“I went from perfectly healthy to being at death’s door.”
– Jacob Dye, sepsis survivor
What your support funds
Your support will have a transformational impact on improving prevention, survival, and long‑term recovery for people facing sepsis. Longer term, it will improve the physical, psychological and cognitive challenges survivors live with, and lift post‑sepsis survival and quality of life. The potential health and economic benefits are immense.
Funding breakdown:
- Personnel & data management: $2.56m
- Patient & site payments: $2.24m
- Operational costs: $0.13m
“The ability to identify someone early and follow them through with effective care could be transformative for patient outcomes.”
– Associate Professor Naomi Hammond

Stop sepsis. Save lives.
Related Stories

A vision for cancer care – NORTH STAR VNP Cancer Clinical Trials Showcase highlights innovation and progress
Read more
MEDIA RELEASE – Introducing Australia’s premier cancer clinical trials centre NORTH Sydney Trials and Research Van Norton Poche (NORTH STAR VNP)
Read more

Gemma’s story – Expert healthcare staff saved my newborn daughter from sepsis caused by enterovirus
Read more