
Category: Patient stories



April 20, 2026
Carolyn’s story: How advances in cancer care helped her beat cancer – twice
Read more
January 12, 2026
Vivien’s story – From patient to philanthropist supporting cancer research
Read more


November 14, 2025
Julie’s aplastic anaemia recovery story – A rare diagnosis, remarkable care, and a gift of gratitude
Read more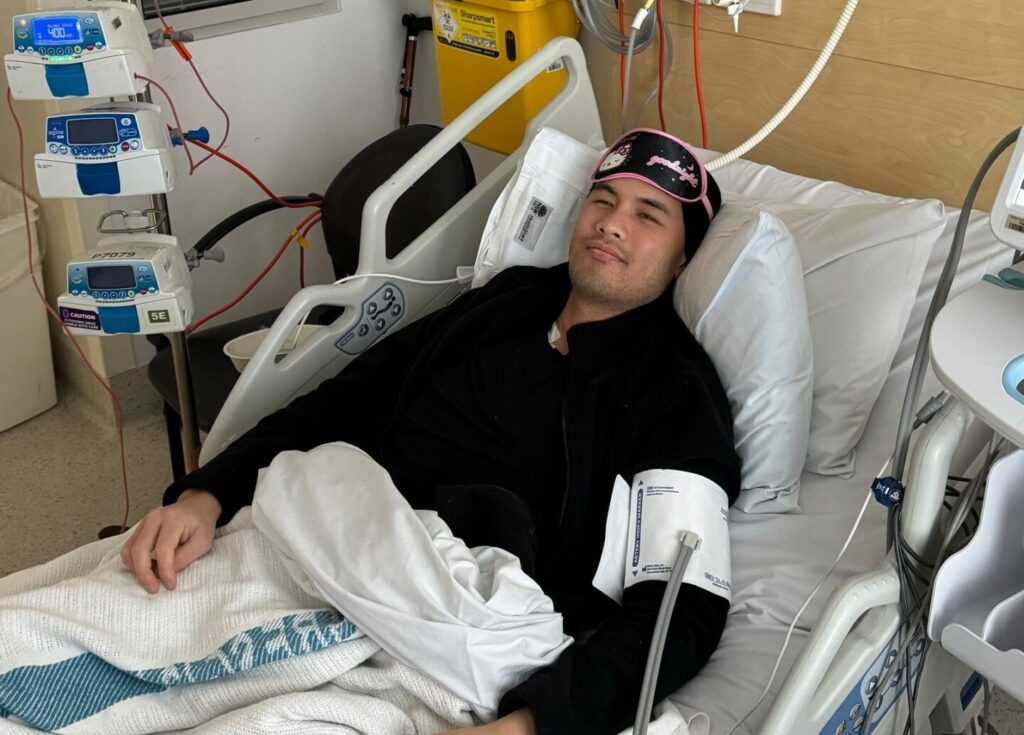

November 04, 2025
Natarajan’s journey – Turning a shocking cancer diagnosis into hope for others
Read more
October 24, 2025
The care that changed everything – How RNSH helped Sharon heal after a severe burn injury
Read more
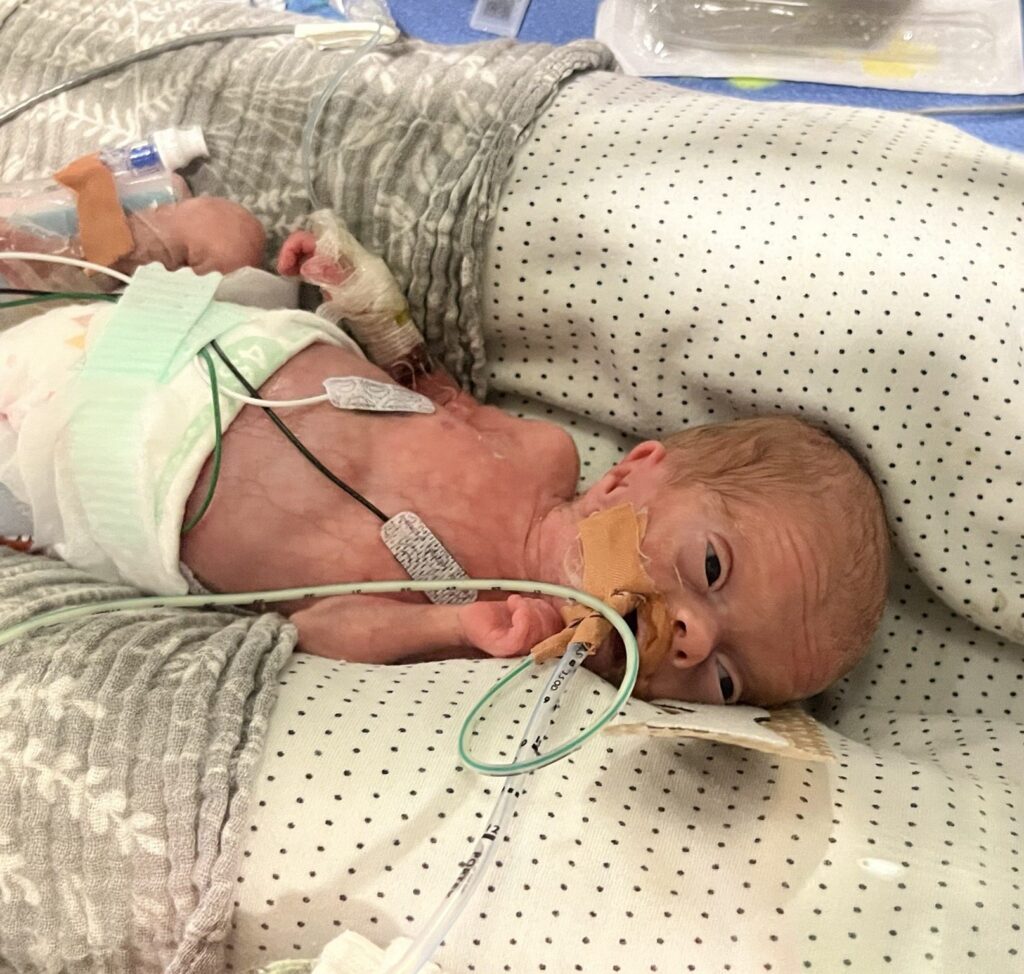
October 24, 2025
A Christmas we’ll never forget – Our premature baby’s time in the RNSH NICU
Read more
Make a Donation
Donate
Subscribe
You can shape the future of healthcare for all
Give a gift that makes a real difference to our healthcare staff and facilities so they can deliver the best patient care.