
Category: Patient stories




April 14, 2025
Christine’s legacy: Supporting brain injury patients and carers through the NORTH Foundation
Read more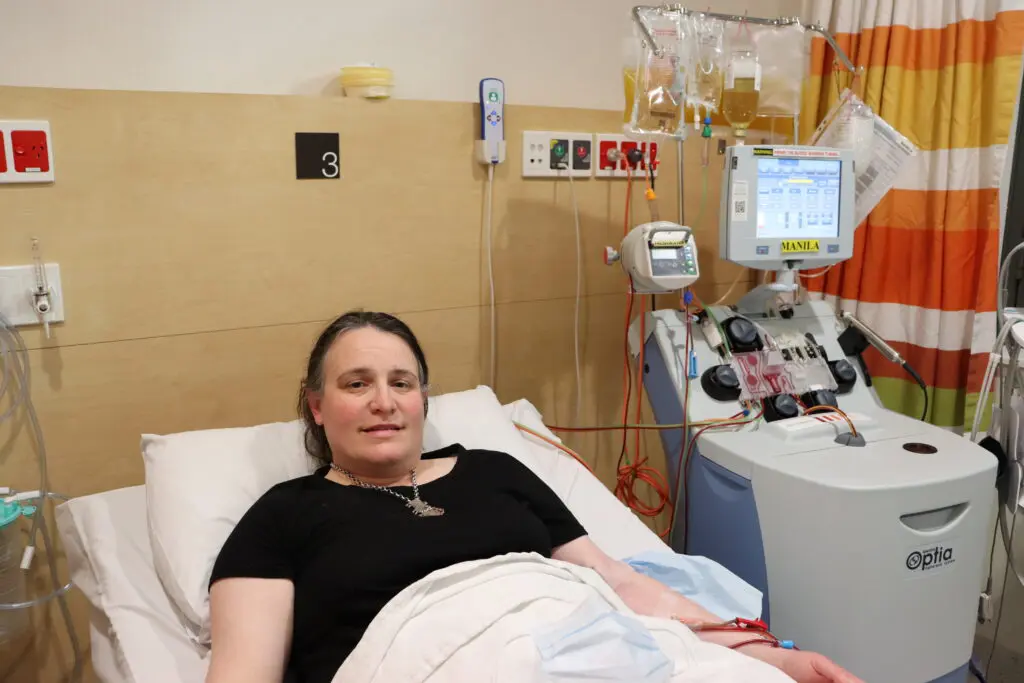
April 10, 2025
Georgina’s story – A testament to exceptional patient care at Royal North Shore Hospital
Read more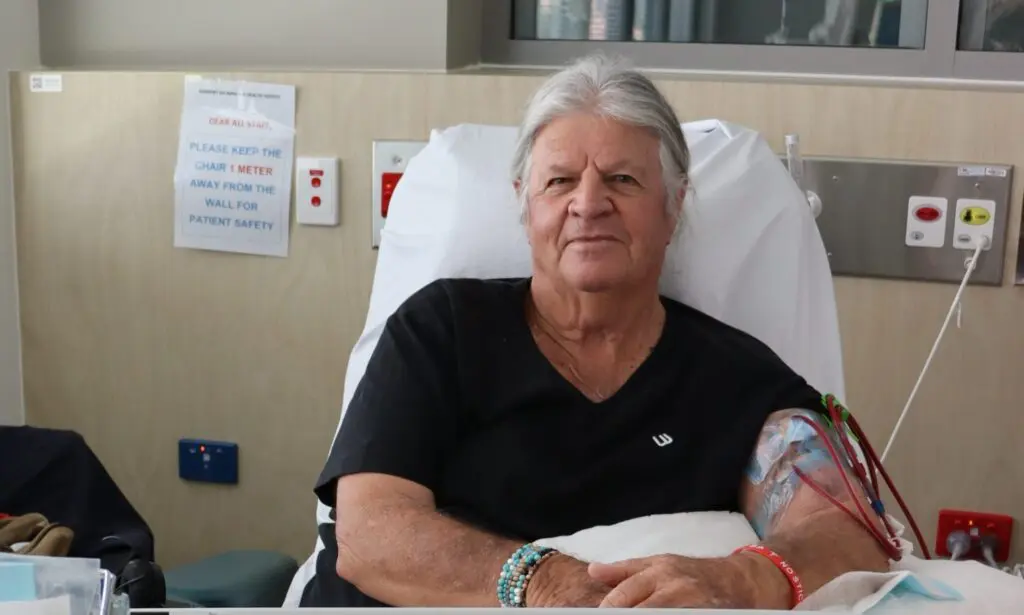
March 12, 2025
Kevin’s journey: How Hornsby Ku-ring-gai Hospital’s new kidney dialysis unit lessens the burden of treatment
Read more
January 19, 2025
Daniel’s journey: overcoming mental health struggles and giving back through the Three Peaks Challenge
Read more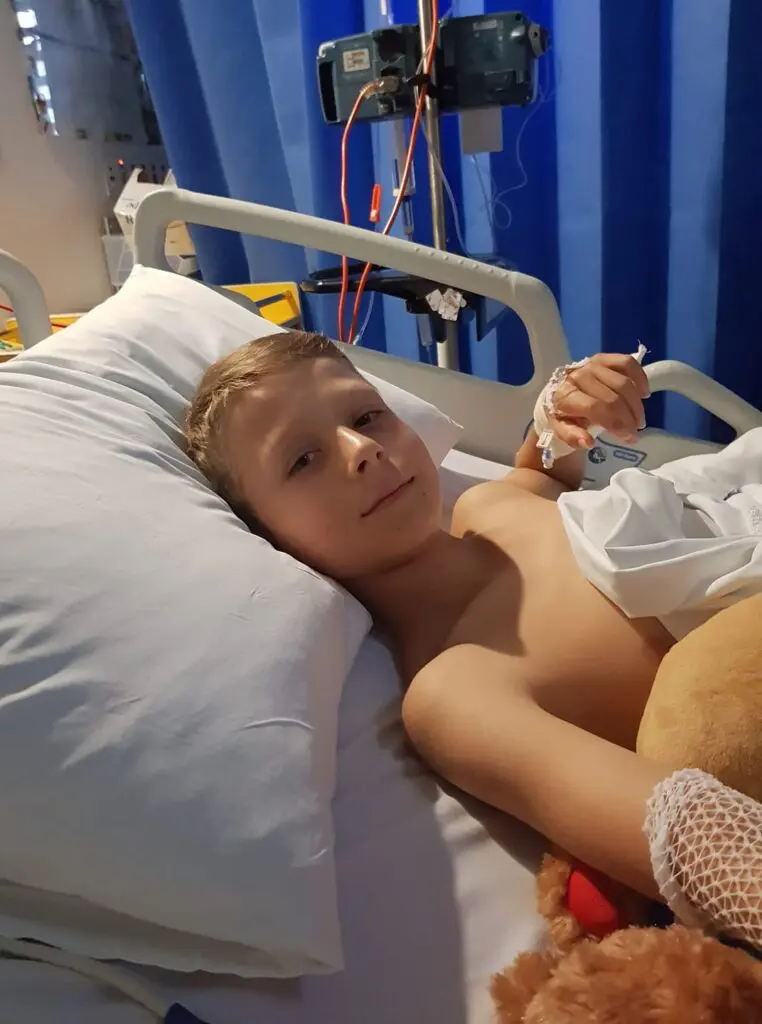
January 19, 2025
Nina’s Story – I show my gratitude for the healthcare staff by donating to the NORTH Foundation
Read more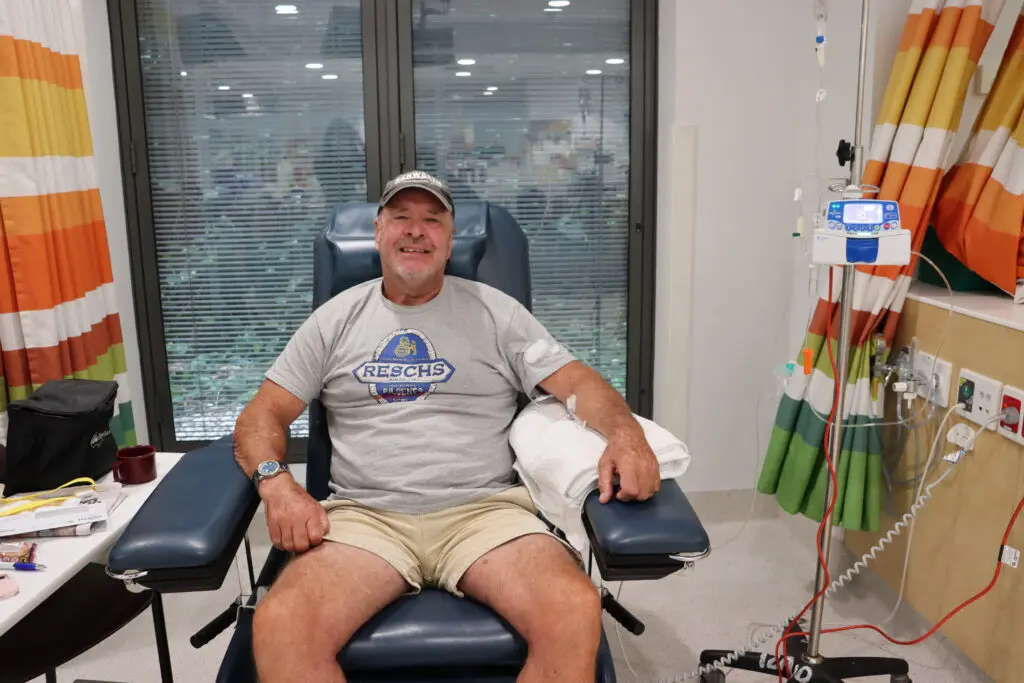
December 10, 2024
Steve’s story – A clinical trial saved my life from aggressive skin cancer
Read more


November 12, 2024
Anil’s living kidney donation journey – A gift for a stranger, a lifeline for my wife
Read more
Make a Donation
Donate
Subscribe
You can shape the future of healthcare for all
Give a gift that makes a real difference to our healthcare staff and facilities so they can deliver the best patient care.