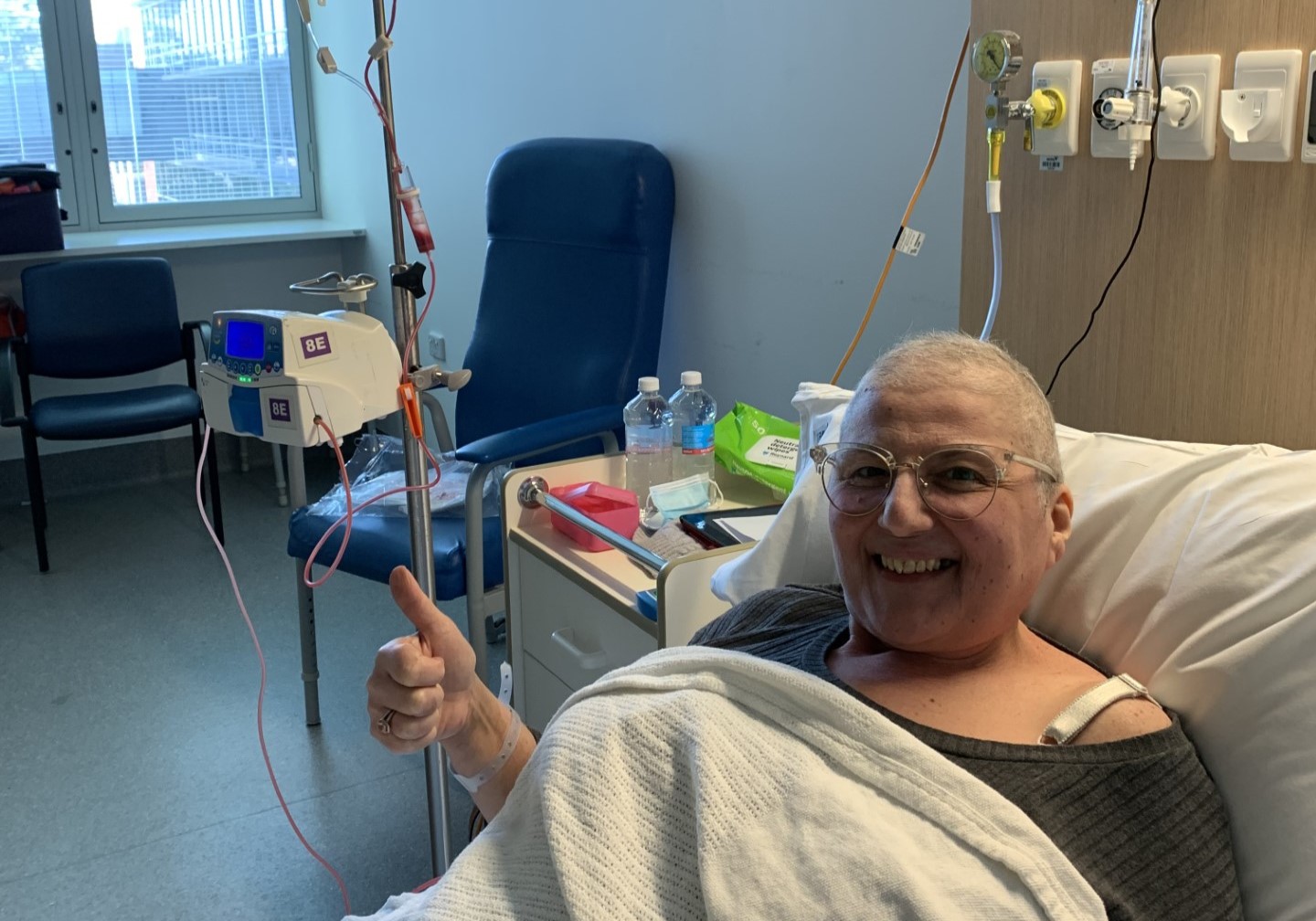
To treat her diagnosis of lymphoma, Margaret received seven gruelling rounds of chemotherapy before a stem cell transplant.
Approximately 6,600 people are diagnosed with B-cell lymphoma each year in Australia.
After working seven days a week for more than 12 years at their fruit shop, Margaret and her husband Vince decided to retire so they could be more available for their growing family. Their three children were now having children of their own, plus Margaret was caring for her 85-year-old mother Antonieta in their home.

Margaret after her recovery
A month later, Margaret was feeling lethargic, was not interested in food and “not herself”. She had noticed a painless swelling on her chest, and she thought it was a fatty cyst. Nevertheless, she went to her local doctor, who ordered an ultrasound scan of the soft tissue.
A few hours following the scan, Margaret received a phone call saying she needed to present herself to the emergency department at Royal North Shore Hospital (RNSH). A doctor informed her that the scans indicated she had several metastatic (or secondary) tumours and she may have pancreatic cancer.
“I was immediately admitted to the oncology ward at Royal North Shore Hospital and during that sleepless night I planned my funeral, music, flowers as I thought it is what it is, and I can’t change it. Watching my family hear my news was worse than being told the diagnosis.”
The next day, Margaret had a biopsy procedure on the soft tissue. She says she was relieved to be told the cancer was not in her pancreas, however she was diagnosed with lymphoma (blood cancer).
“I went from being shocked and devastated at the possibility I had terminal pancreatic cancer, to euphoric as I was told that lymphoma can be treated,” said Margaret.
With further testing, she was diagnosed with large B-cell lymphoma which was a more aggressive cancer of the lymphatic system, an important part of the body’s immune system. She was placed under the care of Professor Ian Kerridge, a haematologist and bone marrow transplant physician at RNSH.
“Professor Kerridge said that we were going to become great friends over the next few years, as he knew I would require long-term treatment,” said Margaret.
At 57 years young and with her loving family and husband beside her, she feels she has a lot to live for. She was enthusiastic about commencing chemotherapy treatment and determined to do exactly what the doctors asked of her to survive her cancer diagnosis.

Margaret volunteering with the Pink Ladies at Royal North Shore Hospital – giving back to the community
After the initial induction chemotherapy, the next phase of Margaret’s treatment plan was a 21-day cycle of intrathecal chemotherapy. High dose chemotherapy was injected directly into her spinal canal during a lumbar puncture, which is where a needle is placed into the cerebrospinal space between two bones (vertebrae) in the spine.
After each cycle, Margaret suffered from a low neutrophil count as chemotherapy targets cancer cells as well as the healthy white blood cells, leaving patients susceptible to infection. The side effects accumulated with each cycle of chemotherapy, and she experienced mucositis or painful ulcers in her mouth and throat in addition to hair loss.
Margaret was incredibly appreciative of the empathy received from her healthcare team and recalls many reassuring conversations with the nursing staff, making her feel safe when she was anxious.
After six courses of chemotherapy, Margaret was advised that she required an autologous stem cell transplant, a form of immunotherapy. While the chemotherapy treatment had been successful, the transplant would use her own healthy blood stem cells to fight off any remaining lymphoma cells, increasing the chances of longer lasting remission.
As Margaret started to prepare for the transplant, she was experiencing high grade fevers and nausea. As her blood pressure was dangerously low, she was admitted to the intensive care unit (ICU) of RNSH.
“I was looked after like the Queen in ICU. During my whole journey, the healthcare staff were wonderful,” said Margaret.

Margaret recovering with with her family including her mother Antonieta
Margaret prepared for the stem cell procedure by self-administering a course of injections to boost the number of stem cells into her bloodstream. A series of procedures followed where blood was collected from Margaret and the stem cells were separated in a process called apheresis. The healthy stem cells were then treated and preserved ready for the transfusion.
Margaret received her seventh and final course of chemotherapy in preparation for the harvested stem cells to be transfused into her bloodstream.
Once discharged, it took Margaret six weeks to recover from the intense treatment. Margaret was elated when a Positron Emission Tomography (PET) scan showed there was no presence of tumours or lymphoma remaining.
Margaret’s beloved mother Antonieta had also been diagnosed with another form of blood cancer – chronic myeloid leukemia (CML) – but due to innovative treatments was able to manage this well for many years. Margaret and her family are forever grateful for life saving research and the opportunity for their mother to be part of trial CML treatments which were successful.
Antonieta unfortunately passed away due to other health complications in January 2023 on what would have been her 87th birthday.
Grateful for the care she received at RNSH and from Professor Kerridge, Margaret generously donated to the RNSH haematology department through the NORTH Foundation to support medical research into new cancer treatments.
If you are grateful for the healthcare you or a loved one received, you can donate towards an area of medicine that matters to you through the NORTH Foundation.

